
Unilateral Vestibular Hypofunction
When One Inner Ear Stops Pulling Its Weight
Dizziness, unsteadiness, and blurred vision when you move your head are not things you just have to live with. Your brain can learn to compensate — and the right physiotherapy makes that happen faster.
Unilateral Vestibular Hypofunction (UVH) is one of the most treatable — and most under-treated — causes of chronic dizziness and balance problems. Many patients spend months avoiding movement, taking medication that suppresses symptoms without resolving them, or simply waiting to feel better on their own. At Alleviate Physiotherapy, we specialise in Vestibular Rehabilitation Therapy (VRT): a structured, physiotherapy-driven approach that helps the brain recalibrate and restore stability across our clinics in Etobicoke, Mississauga, Clarkson/Oakville, and Islington.
What is Unilateral Vestibular Hypofunction?
UVH occurs when the balance organs in one inner ear — or the vestibular nerve connecting that ear to the brain — reduce their function or stop working altogether. The result is an asymmetry in the signals your brain receives from each side.
Your brain normally gets equal, matched signals from both the right and left vestibular systems. When one side weakens, the brain interprets the mismatch as continuous head movement — even when you stand perfectly still. This is what produces that persistent, disorienting sense of motion or instability.
UVH is Not Just "Dizziness"
Many patients with UVH receive a broad "dizziness" label and general advice to wait it out. UVH is a specific clinical condition with a clear mechanism and a well-evidenced treatment pathway. A proper vestibular assessment identifies the nature and degree of the imbalance — and that assessment is what makes rehabilitation targeted rather than generic.
What Causes UVH?
Several conditions can reduce function in one vestibular system. The most common causes your physiotherapist and medical team will consider include:
Vestibular Neuritis
A viral infection that inflames the vestibular nerve, causing sudden and severe vertigo. It often resolves partially on its own, but the residual asymmetry frequently requires VRT to achieve full functional compensation.
Labyrinthitis
Viral or bacterial inflammation affecting both the hearing and balance portions of the inner ear. Symptoms include vertigo and hearing changes. The vestibular deficit it leaves behind responds well to structured rehabilitation.
Acoustic Neuroma Resection
Surgical removal of a benign tumour on the vestibular nerve causes a sudden, complete loss of function on that side. Post-surgical VRT is essential — early rehabilitation significantly improves speed and completeness of compensation.
Ménière's Disease & Other Causes
Recurrent episodes of Ménière's disease can progressively reduce vestibular function over time. Other causes include head trauma, ototoxic medications, and vascular events affecting the inner ear blood supply.
Signs You Shouldn't Ignore
UVH symptoms vary in severity, but they share a common thread — they worsen with head movement and improve with stillness. If any of the following sound familiar, bring them to a physiotherapist for a proper vestibular assessment rather than waiting for them to resolve on their own:
Vertigo
A strong illusion of spinning or movement — either of yourself or the environment around you. In UVH this is typically most intense in the acute phase and may reduce over time, but compensation rarely completes without active rehabilitation.
Ménière's Disease & Other Causes
Blurred vision or a "jumping" of the visual environment when you move your head. This happens because the damaged vestibular system can no longer stabilise your gaze during movement. It makes reading, driving, and busy environments particularly difficult.
Disequilibrium
A persistent sense of being off-balance or unsteady — particularly when walking, turning, or moving through crowded spaces. Falls risk increases significantly, especially in low-light environments where the visual system cannot compensate for the vestibular deficit.
Movement Avoidance & Deconditioning
Many patients restrict head movements to avoid triggering dizziness. This feels protective but actively slows recovery. The brain needs repeated movement exposure to adapt. Avoidance prevents the very stimulus the brain needs to compensate.
4–6
weeks for most patients to achieve meaningful functional improvement with structured VRT
Early
intervention consistently produces faster and more complete recovery than delayed or passive management
VRT
is the gold-standard, evidence-based treatment — not medication or watchful waiting
How Can Physiotherapy Help with UVH?
The inner ear itself may not fully recover. But the brain has a remarkable capacity to compensate — using visual input, joint position sense, and ground contact through the feet to maintain balance in place of the weakened vestibular signal. Vestibular Rehabilitation Therapy drives and accelerates this compensation process.
VRT is not a single exercise or a generic balance programme. It is a structured, progressive set of interventions that your physiotherapist tailors to your specific pattern of dysfunction, symptom severity, and activity goals. What matters is not just which exercises are prescribed, but how they are introduced, progressed, and adjusted based on your response. A therapist-guided programme consistently outperforms self-directed exercise for this reason.
At Alleviate Physiotherapy, we follow our signature three-step approach:
Assess
A comprehensive vestibular assessment — including gaze stability, balance testing, gait analysis, and movement provocation — to map the specific nature of your deficit before treatment begins.
Alleviate
Targeted exercises and strategies to reduce acute symptoms, restore gaze stability, and begin the brain's compensation process in a controlled, progressive way.
Achieve
Progressive balance and functional training to restore confidence, reduce falls risk, and return you to the activities — driving, sport, work — that dizziness has been limiting.
📈
The Painful Arc
Sharp pain when lifting your arm between 60 and 120 degrees of elevation — the zone where the rotator cuff passes under the arch. Pain often eases at full elevation, then returns as the arm lowers.
🌙
Night Pain
Difficulty sleeping on the affected side, or waking from sleep due to a deep, aching pain in the shoulder. Night pain is a consistent feature and often the first symptom patients report.
⚡
Catching Sensation
A feeling of the shoulder “catching” or “clicking” as the arm is lowered from elevation. This is the rotator cuff briefly snagging against the arch as it passes through the impingement zone.
💪
Weakness & Fatigue
Difficulty with overhead activities, reaching behind the back, or lifting objects away from the body. The pain and disuse lead to progressive rotator cuff weakness over time if not addressed.
Treatment Approaches — Guided by Your Therapist
Gaze Stabilisation Exercises (Adaptation)
These exercises use a principle called "retinal slip" — the brief blurring of a target when the head moves — to stimulate the brain to strengthen its balance reflex. A common starting exercise is the X1 viewing paradigm: focus on a stationary target (such as a letter on a wall) while slowly moving your head from side to side. The brain detects the error signal and adapts its response. Your therapist determines the appropriate speed, range, and duration based on your current level of vestibular function.
Habituation Exercises
Certain movements — bending forward, rolling over in bed, turning quickly — trigger dizziness in UVH. Habituation involves repeated, controlled exposure to these provocative movements. Each repetition sends the brain a signal that the movement is not dangerous. Over time, the brain reduces its dizzy response. Your therapist selects which movements to habituate first and how to progress intensity — doing too much too soon can worsen symptoms rather than improve them.
Phase 2: Restoring Balance and Functional Movement
Static and Dynamic Balance Training
Your therapist introduces progressive balance challenges — standing on foam surfaces, reducing visual input, performing dual-task activities — to train your brain to integrate the available sensory signals more effectively. The progression follows your response to each level of challenge. Advancing too quickly without adequate stabilisation at each stage reduces the quality of the adaptation stimulus.
Gait and Walking Rehabilitation
UVH affects walking confidence and safety — particularly on uneven surfaces, in crowds, or in dim lighting. Your therapist works on head movement during walking, turning strategies, and exposure to challenging environments. These exercises rebuild the automatic postural responses that UVH has disrupted and directly reduce your risk of falls.
Sensory Substitution Training
Where vestibular input remains permanently reduced, the brain learns to rely more on vision and proprioception (the sense of body position through joints and muscles). Your therapist guides specific exercises that strengthen these alternative pathways — building a compensation strategy the brain can use reliably in daily life.
Phase 3: Functional and Activity-Specific Rehabilitation
Activity-Specific Exposure and Graded Return
Recovery from UVH is most complete when rehabilitation targets the specific activities your symptoms have disrupted — driving at night, playing sport, working in a busy environment. Your therapist designs graded exposure tasks that progressively reintroduce these demands. This moves rehabilitation from the clinic into your real life.
Falls Risk Management and Home Safety
For patients with significant disequilibrium, your therapist assesses your home environment and daily routines to identify falls risks. Practical modifications and targeted balance exercises reduce your exposure to dangerous situations while the compensation process continues to develop.
Education and Pacing
Understanding what is happening in your vestibular system changes how patients engage with recovery. Your therapist explains the compensation process, sets realistic expectations for the recovery timeline, and teaches you how to manage symptom fluctuations. This reduces anxiety around dizziness — which itself amplifies symptoms — and builds confidence in movement.
⚠ On Vestibular Suppressant Medications
Medications such as meclizine, diazepam, or prochlorperazine reduce the sensation of dizziness in the short term. However, they also suppress the very neural signals the brain needs to drive compensation. Used beyond the acute phase, these medications actively slow recovery. If a clinician has prescribed vestibular suppressants on an ongoing basis, discuss the role of active VRT with your physiotherapist and medical team. In most cases, reducing medication and beginning structured rehabilitation produces better long-term outcomes.
When Should You See a Physiotherapist?
Many people with UVH wait months before seeking vestibular physiotherapy. They assume dizziness will resolve on its own, or they receive medication without rehabilitation. Some level of spontaneous improvement does occur — but without active VRT, compensation frequently remains incomplete. Symptoms that could resolve fully instead become chronic.
Book a vestibular assessment if any of the following apply:
- Dizziness or vertigo that started after a viral illness, head injury, or ear surgery.
- A persistent sense of unsteadiness or imbalance — particularly when walking, turning, or in busy environments.
- Blurred vision or visual instability when moving your head.
- Dizziness that worsens with head movement and eases when you remain still.
- A diagnosis of vestibular neuritis, labyrinthitis, or acoustic neuroma — with or without surgery — where vestibular rehabilitation has not yet begun.
- Avoidance of activities — driving, sport, crowded spaces — because of dizziness or fear of falling.
- Symptoms that have persisted for more than two to four weeks without clear improvement.
You Don't Have to "Just Live With" Dizziness
UVH responds well to structured physiotherapy. The brain's ability to compensate does not disappear — but it needs the right stimulus to do so, and it needs it to come in the right sequence and at the right intensity. A vestibular physiotherapist provides exactly that. The sooner assessment and rehabilitation begin, the more complete the recovery tends to be.
Your Balance Can Improve — With the Right Support
Dizziness and unsteadiness have a cause. Finding it — and giving your brain the structured stimulus it needs to compensate — is what makes the difference between managing symptoms and actually recovering. Our vestibular physiotherapists will assess your balance system thoroughly and build a programme designed around your specific deficit and goals.
Conveniently located across four GTA locations — Etobicoke, Mississauga, Clarkson/Oakville, and Islington.
Reference: Herdman, S.J. & Clendaniel, R.A. (2014). Vestibular Rehabilitation, 4th ed. F.A. Davis Company. | Copyright © 2025 Alleviate Physiotherapy.
-
 Bicep Tendonitis: Physiotherapy and Chiropractic Care
Bicep Tendonitis: Physiotherapy and Chiropractic CareBicep Tendonitis: Physiotherapy and Chiropractic Care Pain in the upper arm? If you’re suffering from Biceps Tendonitis, you should consider...
-
 Frozen Shoulder
Frozen ShoulderFrozen Shoulder Frozen Shoulder also known as Adhesive Capsulitis is a common condition and we at Alleviate Physiotherapy can help...
-
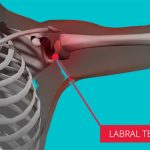 Labral Tears
Labral TearsLabral Tears Labral Tear: Shoulder Pain and Instability Alleviate Physiotherapy is the home to Shoulder Pain rehabilitation. Our clinics located...
-
 Rotator Cuff Dysfunction
Rotator Cuff DysfunctionRotator Cuff Dysfunction Suffering from a Rotator Cuff Injury can be challenging and Alleviate Physiotherapy specializes in shoulder joint rehabilitation....
-
 Shoulder Bursitis
Shoulder BursitisShoulder Bursitis It is one of the most common causes of Shoulder pain and inflammation? Shoulder Bursitis is one condition...
-
 Shoulder Impingement
Shoulder ImpingementShoulder & Upper Limb Injuries Understanding Shoulder Impingement Syndrome Why Your Arm Might Be “Catching” — and What To Do...
-
 Shoulder Pain
Shoulder PainShoulder Pain Shoulder pain can be caused by a lot of reasons and may lead to difficulty in mobility and...











