
Baker’s Cyst
That Mystery Lump Behind Your Knee
A Baker’s cyst is rarely the real problem — it is your knee telling you something is wrong on the inside. Finding out what that is, and addressing it properly, is the only way to make the cyst go away for good.
A lump behind the knee can be an alarming discovery. For most adults, it turns out to be a Baker's cyst — a fluid-filled sac that is not dangerous in itself, but is almost always a sign of an underlying knee joint problem that needs proper attention. At Alleviate Physiotherapy, we treat Baker's cysts by focusing on what is actually causing the fluid to accumulate — not just the cyst itself.
What is a Baker's Cyst?
A Baker's cyst — also known as a popliteal cyst — is not a growth or a tumour. It is a collection of synovial fluid (the joint's natural lubricating fluid) that has become trapped in a small bursa at the back of the knee, located between the medial head of the gastrocnemius (calf muscle) and the semimembranosus tendon of the hamstring.
The mechanism is straightforward: when something inside the knee joint triggers excess fluid production, that fluid finds its way into this bursa through what functions like a one-way valve. Fluid leaks in from the joint but cannot return, causing the sac to fill and distend — producing that characteristic feeling of tightness or a "trapped balloon" behind the knee.
The Cyst is a Symptom, Not the Diagnosis
This is the single most important thing to understand about Baker's cysts: the cyst itself is not the underlying problem. It is the knee joint's response to a problem elsewhere inside the joint. Draining or removing the cyst without identifying and treating the underlying cause almost always results in the cyst returning — sometimes more than once. A proper clinical assessment of the knee is essential before any treatment plan for the cyst is decided.
Why Did the Cyst Form?
In adults, Baker's cysts are almost always secondary — meaning they develop as a consequence of an existing problem within the knee joint. Research indicates that the large majority of Baker's cysts in adults are associated with internal knee pathology, most commonly:
82%
of adult Baker's cysts are associated with a meniscal tear — most often the posterior medial meniscus
↑ Risk
increases with age, as degenerative joint changes become more common and joint fluid production increases
Other conditions that can trigger excess synovial fluid production and lead to cyst formation include:
Meniscal Tears
The most common underlying cause. A tear in the posterior portion of the medial meniscus disrupts normal joint mechanics and triggers an inflammatory fluid response. The cyst will typically not resolve until the meniscal pathology is appropriately managed — whether conservatively or surgically.
Osteoarthritis
Degenerative changes to the cartilage surfaces of the knee stimulate ongoing synovial inflammation and fluid production. Baker's cysts associated with arthritis tend to be chronic and recurrent unless the arthritis itself is well managed.
Rheumatoid & Inflammatory Arthritis
Significant ligament injuries — particularly ACL tears — produce acute and sometimes chronic joint effusions. If the joint continues to produce excess fluid following injury, a cyst can develop in the popliteal bursa over time.
In Children, the Picture is Different
In children and adolescents, Baker's cysts are far less commonly associated with internal joint pathology. They are usually idiopathic — meaning no specific cause is found — tend to be asymptomatic, and frequently resolve on their own without treatment. A physiotherapy or medical assessment is still worthwhile to confirm the diagnosis and rule out anything that warrants attention, but the clinical approach in children is generally more conservative and observational.
Signs You Shouldn't Ignore
Baker's cysts can range from a subtle background awareness to a genuinely disabling tightness. The key point is not the size of the cyst — it is what is causing it. Any of the following warrants a proper knee assessment, not watchful waiting:
- Visible or Palpable Lump: A noticeable mass or fullness at the back of the knee, often more prominent when the leg is fully straightened.
- Tightness or Pressure: A sensation of tightness or restriction behind the knee that limits how far you can bend or straighten the leg comfortably.
- Aching or Discomfort: A dull ache behind the knee that worsens with prolonged activity, stairs, or full range of motion movements.
- Swelling Around the Knee: General knee effusion (swelling within the joint) that frequently accompanies the underlying cause of the cyst.
- Mechanical Knee Symptoms: Clicking, locking, giving way, or catching in the knee — signs that point strongly to an internal joint problem such as a meniscal tear.
- Calf Pain or Swelling Following a Known Cyst: If you have a Baker's cyst and develop sudden calf pain, tightness, or swelling — seek medical attention promptly. See the rupture warning below.
🚨 Cyst Rupture — A Symptom That Requires Urgent Medical Assessment
If a Baker's cyst ruptures, synovial fluid disperses into the calf tissues, causing sudden, severe calf pain and swelling that can look and feel virtually identical to a deep vein thrombosis (DVT) — a blood clot. This is known as pseudothrombophlebitis syndrome. Because the consequences of an undetected DVT are serious, a ruptured Baker's cyst must be assessed urgently by a doctor and confirmed with ultrasound or venography to rule out a clot before any other treatment is considered. Do not attempt to self-assess or "walk off" sudden calf pain if you have a known Baker's cyst.
Why Proper Diagnosis is Essential
Because a Baker's cyst is nearly always secondary to another knee condition, identifying that underlying condition is not optional — it is the foundation of effective treatment. A physiotherapy assessment will evaluate your knee mechanics, range of motion, ligament integrity, and meniscal loading. However, imaging is almost always a necessary part of the diagnostic picture.
An MRI is the investigation of choice for Baker's cysts for two important reasons. First, it confirms that the lump is a fluid-filled cyst and not a solid lesion — an important distinction, as solid masses in this region, though rare, require a different clinical pathway entirely. Second, and more importantly for most patients, it identifies the internal knee pathology — such as a meniscal tear or cartilage damage — that is driving the fluid production. Without this information, treatment is based on incomplete data.
🦵
Clinical Assessment
Physiotherapy examination of knee mechanics, joint stability, range of motion, and symptom behaviour
🔍
Imaging (MRI)
🎯
Targeted Treatment
How Can Physiotherapy Help with a Baker's Cyst?
The golden rule of Baker's cyst management is to treat the underlying joint disorder first and foremost. Simply draining the cyst without addressing what is causing excess fluid production almost guarantees recurrence. Physiotherapy plays a central role in this — both in the conservative management of the cyst and its underlying cause, and in the rehabilitation phase following any surgical intervention that proves necessary.
What that conservative management looks like, and in what sequence interventions are applied, depends entirely on what the underlying cause turns out to be. Rehabilitation for a Baker's cyst secondary to a meniscal tear looks different from management of a cyst driven by osteoarthritis or rheumatoid arthritis. This is why your therapist's assessment findings — and the imaging results — must guide the treatment plan, not a generic knee exercise programme.
At Alleviate Physiotherapy, we follow our signature three-step approach:
Assess
A thorough clinical examination of the knee — including joint stability, range of motion, loading patterns, and symptom behaviour — to understand both the cyst and the underlying problem driving it.
Alleviate
Achieve
Treatment Approaches — Guided by Your Therapist
The following outlines the range of interventions your physiotherapist may draw from, alongside the medical and surgical options that may be relevant depending on what the underlying cause turns out to be. The sequence in which these are applied, and how they are combined, is a clinical decision — not a checklist to work through independently.
Addressing the Underlying Joint Condition
This is the starting point — not an afterthought. Your physiotherapist will direct treatment at the identified cause of excess joint fluid, whether that is a meniscal irritation, early arthritis, or ligament instability. This may involve activity modification to reduce joint loading, manual therapy to improve joint mechanics, and specific exercises to reduce the mechanical stresses triggering ongoing inflammation. Without this step, all other treatment is temporary.
A Baker's cyst is your knee's way of signalling that something is wrong on the inside. The earlier that internal problem is identified and managed, the more straightforward treatment tends to be — and the less likely the cyst is to become a persistent or recurrent issue. Do not wait for the cyst to become painful or disabling before seeking assessment.
Book an assessment promptly if any of the following apply:
- You have noticed a lump or fullness at the back of your knee that is new, growing, or changing in character.
- You have tightness or restricted range of motion at the back of the knee that is affecting your daily activities or sport.
- You have mechanical knee symptoms — clicking, locking, or giving way — alongside the cyst, which strongly suggests an internal joint problem requiring investigation.
- You have a known Baker's cyst and symptoms are worsening despite rest or activity modification.
- You have been told you have a Baker's cyst and have not had a physiotherapy assessment of the underlying knee condition.
That Lump Behind Your Knee is Telling You Something
Don't just treat the cyst — find out what is causing it. Our physiotherapists will assess your knee thoroughly, coordinate with your medical team where imaging or specialist input is needed, and build a treatment plan that addresses the root problem — giving the cyst the best chance of resolving for good.
Conveniently located across four GTA locations — Etobicoke, Mississauga, Clarkson/Oakville, and Islington.
-
 ACL Injury – Physiotherapy and Chiropractic Care
ACL Injury – Physiotherapy and Chiropractic CareACL Injury – Physiotherapy and Chiropractic Care What is ACL Injury? ACL stands for Anterior Cruciate Ligament. Wear and tear...
-
 Baker’s Cyst
Baker’s CystKnee Conditions Baker’s Cyst That Mystery Lump Behind Your Knee A Baker’s cyst is rarely the real problem — it...
-
 Iliotibial Band Syndrome
Iliotibial Band SyndromeIliotibial Band Syndrome Pain in the outer thigh that affects your knee? Come visit one of our centers at Clarkson...
-
 Knee Osteoarthritis
Knee OsteoarthritisKnee Osteoarthritis Knee Osteoarthritis Suffering from Knee Osteoarthritis? Come see a Physiotherapist Near You!! Alleviate Physiotherapy isnow located in Oakville...
-
 Knee Pain
Knee PainKnee Pain Knee Pain? Suffering from a painful knee? Sprain/Strain? Osteoarthritis? What is Knee Pain? Any swelling, locking, popping, instability...
-
 LCL Injury
LCL InjuryLCL Injury Having a bad knee? It could be one of your ligaments. Come visit Alleviate Physiotherapy at Clarkson (...
-
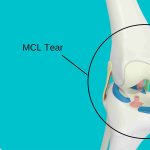 MCL Knee Ligament Injury
MCL Knee Ligament InjuryMCL Knee Ligament Injury Had a recent sports injury to the knee? Come to one of our clinics for a...
-
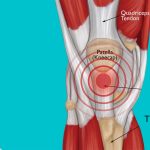 Patellar Tendonitis
Patellar TendonitisPatellar Tendonitis Physiotherapy for Patellar Tendonitis aka Jumper’s Knee Are knee extensions painful? Can’t pin-point your knee pain to a...
-
 PCL Injury
PCL InjuryPCL Injury Have a PCL Tear? Here’s how top-rated physiotherapy can help Suffering from a painful knee? Sprain/Strain? Osteoarthritis? What...











